It’s not just ‘A Little Leak’ – Let’s Talk Women’s Pelvic Floor Health, Treatments, & Solutions
Thanks to leva for sponsoring this post in order to initiate an open discussion about pelvic floor health and bladder leakage, a common problem affecting over 20 million women’s urinary health.
Can’t control your bladder? You are not alone!
Have you had a baby? Roughly fifty percent of women will experience some kind incontinence or pelvic floor weakness within the first year of giving birth and up to 1/3 to 1/2 will continue to have these problems five years later.1
But, it is not just a postnatal problem. High impact sports and prolapse can also lead to a weak pelvic floor. Accordingly, there is a lot of Google-advice for pelvic floor exercises and solutions. Although, a lot of women are not sure how to do them or if they are doing them correctly or effectively. If you are having ongoing symptoms of pelvic floor weakness it is time to find a solution.
There are many causes of bladder leakage due to weakened pelvic floor muscles. Some of the more common are:
- Childbirth
- Increasing age
- Hysterectomy
- Diabetes
- Menopause
- Elevated BMI
What are your symptoms? Take this quiz to rate your bladder health and get your pelvic score.
WHY? WHY? WHY?
After you innocently walk up a flight of stairs, laugh a little too hard, or have to excuse yourself to sneeze it may not seem fair. Incontinence is, at the least, inconvenient but, especially when it surprises you, it can be desperately frustrating.

On the whole, there are a lot of reasons that urinary incontinence can affect a woman. In fact, they run the gamut from childbirth to menopause and anything that causes structural problems. Likewise, medical issues like diabetes, Parkinson’s, MS, tumors, and/or obstructions can also be the culprit. And, as if that were not enough reasons, it could also be a reaction to something you have eaten, drank, or a medication.6
Urinary Incontinence (UI) is generally lumped into one of a few categories but can also be a combination of types3:
- Stress – This is the most common type in women and is caused by putting physical stress on the bladder. Actions such as sneezing, laughing, bending, lifting, or coughing.
- Urgency – Also referred to as overactive bladder. Highlights include an uncontrollable flow of urine and feeling the need to go to the restroom – even when you just went. This can be caused by nerve or muscle damage.
- Overflow – A person experiencing Overflow Incontinence will often unknowingly leak or dribble because the bladder never fully empties.
- Functional – Functional Incontinence is most commonly seen in the elderly and people who cannot move quickly or communicate their need to go to the bathroom.
SOLUTIONS FOR YOUR PELVIC FLOOR HEALTH
Please discuss all options with your doctor before embarking on any sort of self-diagnosed therapy. Those listed below are designed to be used as part of a wholistic treatment program and do not take the place of a professional. You and your doctor can decide which option or options will likely provide you with the best results for your situation.
BEHAVIOR MODIFICATION
This is likely where you will begin if your causes are suspected to have a solution that can be found by making lifestyle and behavior changes. If you suspect a certain food or drink may be the culprit start a diary and begin an elimination diet to narrow down the cause.
Foods that often irritate the bladder:
- Caffeine
- Alcohol
- Spicy Foods
- Carbonated Beverages
Likewise, if you can link your symptoms to a medication you and your doctor can look into other options.

Another way you may begin this journey is by looking into your routine and habits. How much liquid are you drinking? When are you drinking and does changing that help or increase symptoms? Are you overweight? The extra weight can put pressure on your pelvic floor.
Oh, yeah, and stop smoking – this leads to chronic coughing and coughing leads to leaking and then we are back to the beginning.
PHYSICAL THERAPY & EXERCISE
Much like working your body for health you can often subdue or eliminate UI by working out the muscles in your pelvic floor.2 Making them stronger and more focused can help you have more control over your urine flow. Kegels are the most well known but there are many specific exercises that will improve your overall pelvic floor health that are less obvious. A physical therapist can guide you because, at the end of the day, doing them correctly is the key to seeing results.
This is a great place to introduce the amazing marriage of modern medicine and technology by working with your doctor to utilize an intravaginal device like leva, to ensure you are getting the most out of your efforts.
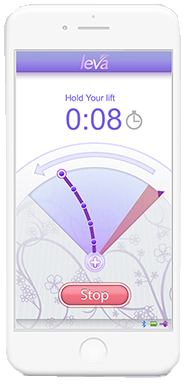
There’s an app for this!
leva is a personal FDA-approved pelvic floor muscle trainer with real-time interactive visualization. It involves no surgery or medication and only takes 2 ½ minutes, twice a day. The accelerometer connects easily to your smartphone to display your progress, mirroring the motion of your pelvic floor. This way you can visibly see that you’re doing the exercises correctly. There is coaching to help you track, review, and easily share your data and experience with your doctor. And, the best part, it works! 87% of women reported no leakage in just six weeks of using leva.
How great will it be to work towards a solution from the privacy of your own home?!
MEDICATIONS, SURGERY, & PROCEDURES
Less invasive options tend to have a great success rate. Sometimes, like training any muscle, it may take some time to see results. Up to a year is not uncommon. However, once you have exhausted those options your doctor may help you find relief through the use of slings, Botox injections, sacral nerve stimulators, and/ or medications. These are provided exclusively by your doctor with whom you will discuss alternatives for your situation.4

WOMEN’S PELVIC FLOOR HEALTH IS QUALITY OF LIFE HEALTH
Bladder leakage and problems associated with it rarely improve over time. Moreover, early treatment provides the best results and gets you back to your lifestyle as soon as possible.
Not discussing your pelvic floor is the only option that will give you no results. Start by talking with your doctor or even a friend. Further, if you would feel more comfortable with someone who deals exclusively with women search for a urogynecologist. Their practices are focused exclusively on treating women’s pelvic floor health and urinary incontinence.
As the great, Reba McEntire said, “All the money in the world can’t buy you back good health.” So, protect it by being proactive. Your health is important.
Learn more from our Sources:
1. Schlosberg, Suzanne and Tracey Zemitis. “Your Guide to Urinary Incontinence After Childbirth.” Parenting, https://www.parents.com/pregnancy/my-body/postpartum/urinary-incontinence/.
2. “The Secrets of the Pelvic Floor.” Goop, https://goop.com/wellness/sexual-health/the-secrets-of-the-pelvic-floor/.
3. Markland, Alayne D., Holly E. Richter, Chyng-Wen Fwu, Paul Eggers, and John W. Kusek. “Prevalence and Trends of Urinary Incontinence in Adults in the United States, 2001 to 2008.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3197263/.
4. Gavin, Kara. “Nearly Half of Women Over 50 Experience Incontinence, but Most Haven’t Talked to a Doctor.” University of Michigan Health Lab. https://labblog.uofmhealth.org/rounds/nearly-half-of-women-over-50-experience-incontinence-but-most-havent-talked-to-a-doctor.
5. “Urinary Incontinence: What you need to know.” MedicalNewsToday. https://www.medicalnewstoday.com/articles/165408.php.
6. Chao, Jamie H. “8 Causes of Urinary Leaks and 8 Ways to Stop Them.” Aurora Health Care. https://www.aurorahealthcare.org/patients-visitors/blog/8-causes-of-urinary-leaks-and-8-ways-to-stop-them.
7. PelvicScore.com.
8. The leva Pelvic Digital Health System. https://www.knowleva.com/.








